How are you going to attract future generations to join your workforce? Experts recommend these best practices:
- Be purpose- or mission- driven
- Listen to your staff
- Empower workers with some level of autonomy
- Be a diverse and inclusive organization.
Blogger Alaina Love, chief operating officer and president of Purpose Linked Consulting, in a recent post on Smartbrief.com, outlines what Generation Z—individuals born between the mid-1990s and mid-2000s—is looking for in their work and their careers.
According to Love, research backs her assertion that Gen Zers are “among the most purpose-, passion- and values-driven talent cohort in the workforce.” This is evident in how they make purchasing decisions, what they seek in their employers and the direction of their career trajectories.
In fact, a recent Deloitte study of Gen Zers and millennials—those born in the early 1980s through the mid-1990s—found that both generations want business leaders “to take the lead in solving the world’s problems, to shift organizations’ motives from inordinately focusing on making profit to balancing social concerns, and to be more diverse, flexible, nurturing of and generous with its employees.”
In other words, organizations that meet these criteria will attract and retain the best of both generations and be better for it. How so? Love cites yet another recent survey of Gen Zers, in which half of the respondents are influenced in their purchasing by “a brand showing dedication to social impact, by giving proceeds to charity, being environmentally conscious, having strong values, or projecting an impact-driven image.”
Find your why
The evidence for becoming a purpose-driven organization is more overwhelming today than ever before. And one proven way to make purpose a priority is to discover your organization’s “why”—as in, why your company exists and why it does what it does. Known for delivering one of the business community’s most popular TED Talks, Simon Sinek has helped thousands of companies and millions of people identify their whys.
As a senior living provider, whether you are for-profit or not-for-profit, finding your why is an imperative that yields many benefits. In most cases, your why is not your official mission statement. Rather, it’s a simple, yet compelling statement that stimulates buy-in from others. An authentic why helps you maintain perspective, build a positive corporate culture and create a trustworthy organization that is connected to a purpose-driven business.
What’s more, living that why will help you attract others who are driven by purpose, inclusiveness, diversity and empowerment. As Love notes, next year, Gen Z will comprise 32 percent of the population, surpassing millennials as the most populous generation. How prepared is your organization?
To learn more about how Quantum Age can help you identify, cultivate and execute your why, contact us.

 believes that while “the updated measures give prospective nursing home residents and their families more information when choosing a facility, they do little to ‘impact the accuracy and reliability of the measures reported.'"
believes that while “the updated measures give prospective nursing home residents and their families more information when choosing a facility, they do little to ‘impact the accuracy and reliability of the measures reported.'"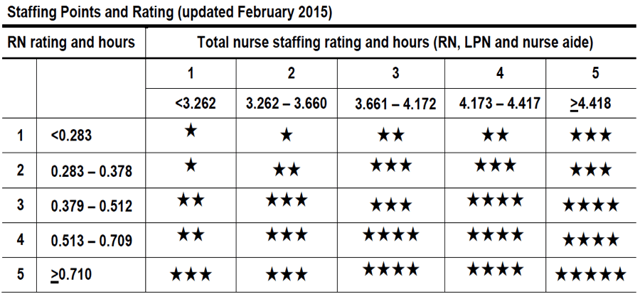
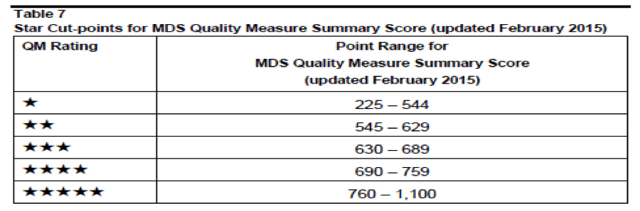

 example.
example. This assertion is not a new one for Thomas, who had just finished his
This assertion is not a new one for Thomas, who had just finished his  is of our own creation. We manufacture disability, frailty, weakness, and we create it on a massive scale.”
is of our own creation. We manufacture disability, frailty, weakness, and we create it on a massive scale.”